One of the first lung transplant patients to receive a skin patch from his organ donor in a trial says it has been ‘invaluable’ in identifying rejection before any other symptoms.
Early warning system
The SENTINEL trial was set up to investigate if skin patches can be used as an early warning system to identify if lung transplants are being rejected. This means treatment can begin sooner, reducing the chance of permanent lung damage.
Lung rejection occurs when the transplanted organ is attacked by the immune system. Lung rejection is difficult to detect and involves frequent hospital visits with invasive blood tests, bronchoscopies, lung biopsies and X-rays. Rejection rates are highest in the first 3-6 months after a transplant and involve up to 30% of patients.
Only half of lung transplant patients are still alive after five years, with rejection a significant factor in deaths post transplant.*
Patches of skin could detect rejection
Transplanting patches of skin with lung transplants may detect rejection by showing as a rash on the donated skin patch and may prevent the body rejecting the lungs. If such a rash is seen, a small biopsy from the skin will be taken, as a step to confirm the presence of rejection.
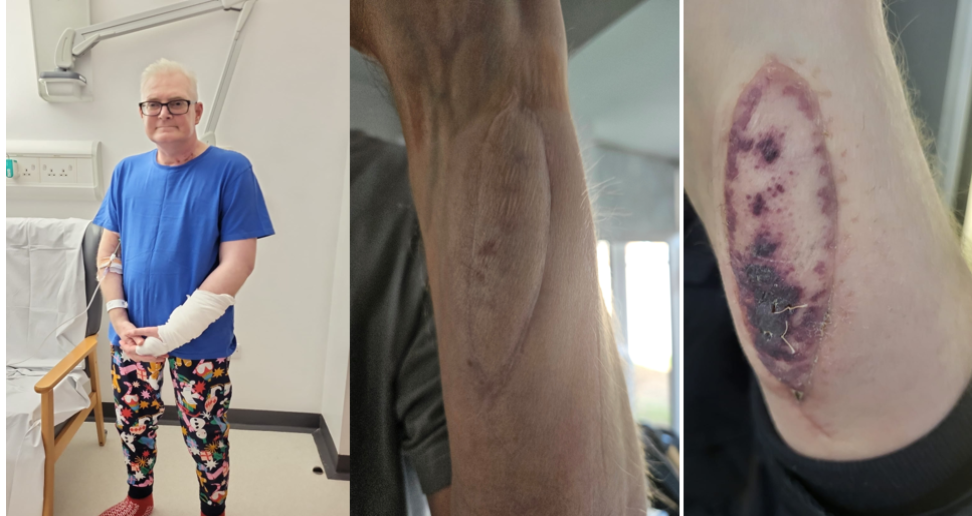
Darren White, 53, dad to Daniel, aged three, was one of the first patients in the UK to receive a skin patch as a part of the SENTINEL trial and believes it has been critical in identifying early rejection of his transplanted organ after his patch developed a purple rash.
He was under the care of the University Hospital of North Tees then referred to Newcastle’s Freeman Hospital. The former bus driver received his lung transplant there in late 2024, after being diagnosed with lung fibrosis**, at the start of the year.
“I started to feel more and more breathless, I had to sit down for five minutes after going up the stairs of my bus. I sought medical attention and was sent directly to the hospital. Never did I think that I would get the diagnoses that I did and that I would need a lung transplant”, says Darren.
After two months on the waiting list, Darren, who is married to Karen, aged 50, received the call to say a donor had been found. He had been approached about being a part of the SENTINEL trial, which started in 2024, while he was waiting. He received a patch of skin from his donor, transplanted on to his forearm.
“I didn’t hesitate to say yes”
“I didn’t hesitate to say yes. Anything that might help to avoid rejection was worth a try. Rejection is the biggest fear of any transplant recipient, so having something that might be able to catch it much sooner than otherwise, was really appealing.”
Three months after transplant, Darren, from Stockton-on-Tees, noticed a purple rash on the skin patch and sent photos to his medical team.
He went into his transplant centre for a skin biopsy and results showed very mild rejection, which was treated with steroids. The skin patch empowers patients around rejection fears, allowing them to look out for it and actively take action. Darren responded to treatment and is now doing well.
“I definitely believe the skin patch helped to stop the lungs from being rejected. I was feeling fine, there was no reason for me to think that the lungs were being rejected, the only sign was the rash.
“I’m over a year post-transplant now and doing really well. Who knows if that would be the case if the rash hadn’t shown up and rejection wasn’t spotted until further down the line.
“The trial is a truly fantastic thing and I hope it goes on to show that a skin patch is a viable option for identifying rejection as early as possible. If anybody in my position is approached about the possibility of receiving a skin patch, I’d say absolutely join the trial. Don’t hesitate, just do it.
“The trial is brilliant, it’s helping me looking after myself and it’s given me peace of mind because you can check your skin.”
“Eternally grateful”
“I’m eternally grateful to the trial team but most of all, to my donor’s family, who made the selfless and incredibly generous decision to allow donation to go ahead, but to also agree to this extra donation, of the skin patch. I hope they know how important both of those decisions were to me and how I thank them every day. Thank you, thank you without end.”
Speaking about the overall difference his lung transplant has made, Darren says: “The biggest difference is I can walk, I can take Daniel to the park to play. Before he could sit on my knee, drive my buggy but that was it, I couldn’t do much with him. I can be more of a dad now.
“My favourite thing is to go to the park, Daniel always asks to go on the swing and we have one in our garden. I can push him now. It’s the simple things that are the best, we both love it.”
If the SENTINEL trial is a success and the approach can be rolled out to all lung transplant and heart and lung transplant recipients, the research team believe it could cut lung rejection.
In Newcastle, the trial is led by Andrew Fisher, professor of respiratory transplant medicine at Newcastle University and honorary consultant respiratory physician at Newcastle Hospitals.
“It’s exciting to see patients taking part in the SENTINEL skin patch trial. If successful, this approach has the potential to revolutionise the way lung transplants are performed in the future and reduce the problems with detecting and treating rejection early, which is vital.”

Patients receive a 10 x 3cm skin patch from the forearm of their organ donor, which is transplanted onto the patient’s forearm, at the same time as the lung transplant. The skin transplant is carried out by a plastic surgeons from the University of Oxford as well as the lung transplant centres, working alongside the transplant surgeon.
Skin seems to reject earlier than other organs and is easily visible at all times. This means doctors can treat the rejection as soon as a skin rash appears, to try to prevent the lung from also rejecting.
If the skin flap produces a rash and therefore indicates possible rejection, a skin biopsy can be taken instead of an invasive lung biopsy, which is better for patients as the skin test is less invasive.
Collaborative effort
Attaching the skin transplant requires skilled microsurgery which is performed by plastic surgeons working alongside the transplant surgeon.
In Newcastle, our plastic surgery team has been critical to the running of the trial by both helping with the collection of a piece of skin from donors and then connecting the skin flap to the patient having a lung transplant.
The plastic surgery team monitors patients after the skin transplant procedure and carries out biopsies when needed.
Consultant plastic surgeon and surgical lead, Mr Dan Saleh, has worked with Professor Fisher on the SENTINEL trial. He said:
“This trial would not have been possible without the exceptional collaboration between our transplant and plastic surgery teams, and the support of colleagues from across the microsurgery team at Newcastle.
“The SENTINEL trial is a strong example of our commitment to leading nationally and internationally recognised, pioneering research, and contributing to Newcastle’s history of strong transplant innovation.”
Donor families need to give consent for the skin transplant to take place, which will be requested by NHS Blood and Transplant specialist nurses.
Window to the transplant
Henk Giele, chief investigator of SENTINEL and Oxford plastic surgeon, says “It seems logical that having a window to your transplant can provide an early warning system of rejection or reassure you that you don’t have rejection but we have to prove it works.
“We are so grateful to the patients, the donors and their families, the transplant teams, and the NHSBT staff who make this important trial happen. We hope it will change what we know about transplant and makes patients lives better and longer.”
Emma Lawson, organ donation innovation and research lead at NHS Blood and Transplant, adds: “Thanks to the generosity of amazing donor families providing additional consent for skin grafts, patients are now receiving them and we are privileged to work alongside them to enable this important trial to go ahead. Our specialist nurses in organ donation are supporting families at every step and we continue to match suitable patients for retrieval and transplant.”
Professor John Simpson, director of the MRC-NIHR EME programme, said: “NIHR marks its 20th anniversary this year and during that time, we’ve funded research into a wide range of cutting-edge studies like SENTINEL, assessing innovative new treatments which can help people live healthier lives for longer.
“Research to identify life-changing treatments starts with people like Darren, and with the family of his organ donor. Without his participation, or that of the families who generously donated these additional skin grafts, we couldn’t run this crucial trial.
“Stories like Darren’s have driven the NIHR’s mission over the past two decades, and they remain the reason we continue to fund and deliver research that changes lives today. We encourage everyone – no matter their current state of health – to take part in research by signing up to the NIHR’s free Be Part of Research service.”
Further information
- The £2 million SENTINEL trial is run by the Surgical Intervention Trials Unit as part of the Nuffield Department of Surgical Sciences and sponsored by the University of Oxford in collaboration with NHS Blood and Transplant and the five UK cardiothoracic transplant centres.
- It is funded by a UKRI Medical Research Council (MRC) and National Institute for Health and Care Research (NIHR) partnership.
- Sentinel skin grafts have previously been used in studies where patients received intestinal transplants. It was observed that patients who received a skin patch experienced a much lower rate of organ rejection – around half of what would be expected, suggesting that the patch helped to prevent rejection as well as being a useful monitor of early rejection.
- The trial is set to run until 2027 and will recruit a total of 152 patients. To date, 39 patients have been recruited to the trial and ten patients have received a skin patch.
